A logical model for creating leverage in radiology operations
Over the last decade, practices offering diagnostic imaging have experienced a tremendous explosion in requests for services from physicians, clinics and hospitals for more imaging procedures while requiring increasingly shorter turn-around times for the delivery of results.
MRI scans have tripled in the decade from 1997 through 2006. The increased request in diagnostic services can be attributed to advances in imaging technologies that have had a more positive effect on diagnosis, improving patient outcomes.
There has been a corresponding increase in the number of diagnostic imaging centers to accommodate the growth in demand for diagnostic imaging. With technological changes, expectations have increased from the referring community. Referring hospitals and clinics prefer electronic data exchanges to traditional paper methods. This is particularly true as EMRs and EHRs become more prevalent.
New economic and competitive pressures, along with increased customer intensity, have driven radiology organizations to re-evaluate strategic and operational plans and implement new ways to address these changes.
Some practices may be focusing too much on pursuing “new, new” application technologies— Unified Worklist, Business Intelligence, etc.—without putting the right foundation in place first.
An integrated workflow provides a solid foundation on which to add new applications and deliver innovative services to your referring physician community.
Absent a robust foundation, implementation costs can escalate without realizing tangible results.
What does the right foundation entail?
This paper highlights a systematic approach (see Figure 1 below) to enabling an integrated environment to support innovative initiatives and cost-saving approaches. The result: a radiology practice built for growth and efficiency.
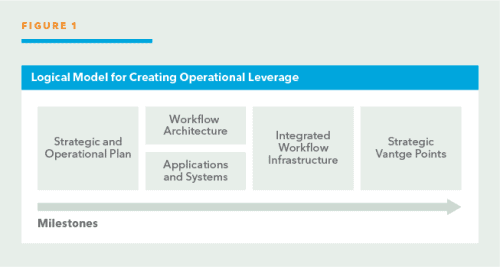
Defining the workflow: key touch points
Before beginning the workflow process, well-defined strategic and operational plans should be available. These plans will drive the radiology workflows that are required as well as the applications and systems to support a streamlined radiology operation. To begin bringing the plans to life, documenting the key workflows necessary to achieve the strategic and operational objectives is an important step.
Understanding the operational value is defined by mapping the workflow architecture end-to-end and identifying any apparent workflow gaps. A strategy to close the identified gaps should be implemented to ensure missing gaps in the foundation do not later cause costly delays. Defining workflow completely can be difficult and complex; however, it will pay big dividends for radiology practices looking to maintain sustained growth and efficiency as they introduce new systems to their IT environments to maintain loyal referring clients and improve customer experiences.
Illustrated in Figure 2 is a sample workflow based on the various roles within an organization.
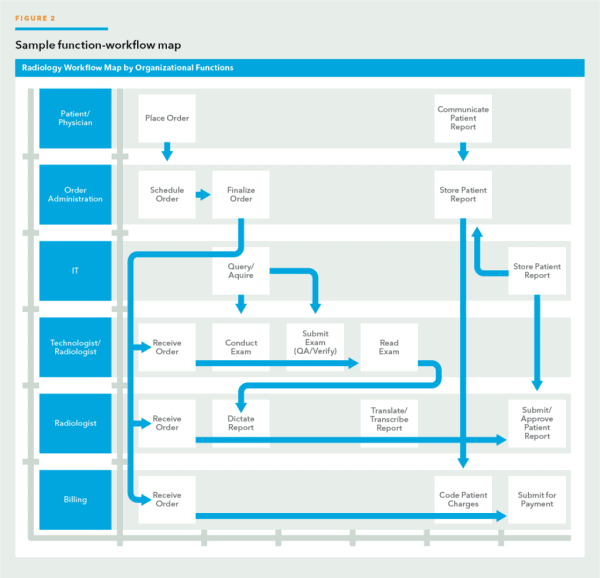
When developing the workflow map there are three primary touch points with major activities that need close attention.
- Customer touch points
Evaluate points in the workflow where patients and referring physicians interact with your practice. Ensure your customer touch points deliver the intended level of service and experience necessary to align with your strategy and positioning in the market. For each of these steps in the workflow, well-defined processes are a plus as well as properly trained team members on what to do. The customer experience is paramount. - Department touch points
Analyze points in the workflow where departments within your practice or group exchange data. This is critical in terms of efficiency and accuracy. Defining the processes and activities will reflect in timeliness and accuracy on patient reports, bills, etc. - Radiologist touch points
Assess points in the workflow where radiologists perform readings and then produce reports, taking in consideration any manual processes that hinder productivity. Reviewing the radiologist procedures ensures the right processes and activities are defined to facilitate greater capacity and capabilities.
Supporting workflows: applications and systems
With the strategic and operational plans and the workflows clearly defined, the stage is set to ensure the right applications and systems are in place to support them. The required applications can vary based on the plans and workflows.
For example, with a specific strategic focus, the required systems approach could be a single RIS, a single PACS, or Dictation/ Voice Recognition (VR) systems. Other plans or workflows may require having multiple PACS systems and having the capability to read remotely for referring clients. The differing characteristics will drive what types of applications are required to support the workflows (see table below).

Whatever the strategic/operational plans and workflows, it is critical to map the workflows to the supporting applications. This will ensure that the applications are in place to support the workflows required to meet the business objectives.
Figure 3 illustrates a mapping of the workflow to the necessary applications.
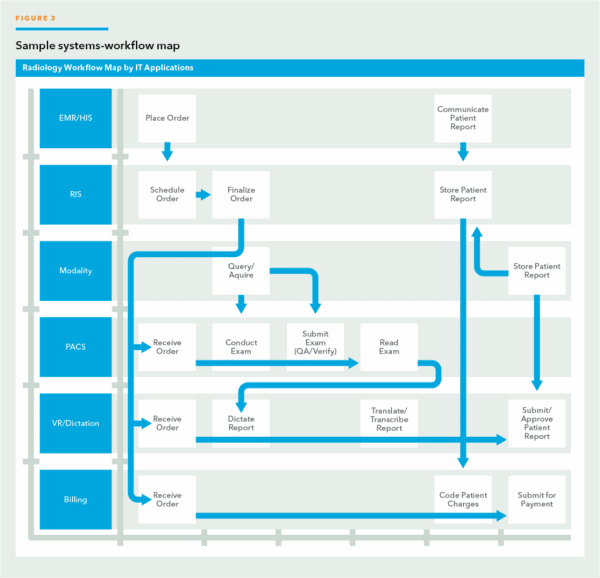
Unifying workflows through integration
Practices that operate in unified, integrated workflow environments have the advantage. The advantage is in the capability to implement applications and systems in a well-coordinated manner that improves enterprise-wide workflows. Radiologists working in an integrated environment generally experience higher productivity, enabling them to deliver greater quality and quantity through the order–to-results cycle.
An integrated workflow infrastructure means having a platform in place to facilitate patient data flow in a seamless, easy-to-manage manner, even with different systems, different data formats, and different interface requirements. Orchestrating the data flow is the central value of integrated workflow infrastructure, commonly driven by an integration engine.
Eliminating or significantly reducing manual effort in workflows is the new standard for radiology groups and departments. Go paperless.
More often now, practices planning for growth discover that point-to-point interface environments are not suitable for adopting new applications and systems to enhance service. This discovery leads to implementing integrated workflow solutions, which will provide enterprise-wide interoperability with systems and applications that operate as a synchronized unit. Beyond reductions in overall cost, patient care and safety are enhanced.
Integrated workflows, using an integration engine platform, ensure the data flow is quick, efficient, and accurate, as formats are adjusted to meet the requirements of each application in the workflow. The integrated workflow and data flow leads to a unified experience—a unified workflow.
Practice-wide results gained are:
- Productive radiologists Radiologists receive the patient data when and where they need it so that they can perform reads in a timely manner.
- Patient report TAT Patient reports are delivered to the referring physician in less time than ever with stat reports often delivered in minutes.
- Accurate, timely billing Billing information is sent electronically to the correct systems so that there is significant efficiency in the processing time and days sales outstanding (DSO) is reduced.
Radiology practices that neglect the benefits of integrated workflow and the enterprise-wide value in a robust integration platform discover lengthy implementation times and higher cost with each new application. To this point, using the 80/20 rule, eighty percent of the tangible value is gained by implementing a solid integration platform that supports an integrated patient data flow, with the remaining twenty percent attainable with the implementation of other strategic initiatives.
Taking the time to put the right pieces in place will deliver real, tangible value while setting the foundation from which to build new strategic vantage points.
Think about setting the foundation this way. It may be tempting to read the last chapter of a thought-provoking novel to see how things turn out. However, by skipping ahead, the storyline may not all fit together and much of the value of the story may be lost.
Unified workflow environment: creating strategic vantage points
Strategic vantage points provide an opportunity for radiology groups or departments to further differentiate and streamline operations.
Several strategic vantage points can be implemented. The strategic vantage points can be placed into three primary categories:
- Worklists
- Operational and workflow metrics
- Physician outreach
Worklists
Worklist solutions on the market are capable of handling substantial volumes of readings efficiently through aggregating data flow from multiple RIS, PACS, and HIS systems. Often adopted by large practices with a wide-ranging multi-site client base, unified worklist offer a scalable solution in solving the issue of physician productivity. Unified worklist solutions coordinate data flow into a single worklist taking into consideration practice subspecialties, group size, workload, and priority of readings.
From a workflow perspective, a unified workflow provides a foundation for radiology practices to launch a unified worklist application more effectively in reducing cost of redundant interfaces to worklist application, proactively monitoring the data flow, and handling all the varying data standards and formats, with complete control in managing the exchange of data to meet each system’s requirements. Without an integration platform, integrating applications to the worklist can be time-consuming.
Operational and workflow metrics
Gaining operational insights is critical for many radiology groups today. Typically, there are three levels of analysis to consider: 1) Immediate through dashboards, 2) Intermediate through operational reporting, and 3) Longer term through business intelligence.
Real-time dashboard
Dashboards are the buzz in healthcare. Gaining instant feedback on 3–6 metrics facilitate removing constraints in the workflows and keeping operations running at near-peak levels. Several radiology dashboards include metrics such as:
- Current turn-around time (TAT)
- Number of studies which have exceeded “normal” TAT threshold
- Patient wait times
Operational metrics reporting
An operations monitoring solution uses the data already flowing through workflows and captures point-in-time snapshots on the health of the operations. It can collect and store operational and workflow data presenting it in meaningful reports based on a given hour, day, or month. Some key operational reports may include:
- Order to result TAT (by hour, day, week, modality, ordering facility, radiologist)
- Complete order cycle TAT – gives more visibility into the duration of each stage of the order cycle (for instance, the time between order being placed and ready to read or ready to read and preliminary result complete)
- RVUs (per radiologist, per shift or hour worked, per referring facility)
- Study volumes (by modality, referring physician, facility, day, week, month)
Business intelligence
In a 1958 article, an IBM researcher first used the term business intelligence (BI). They defined intelligence as “the ability to apprehend the interrelationships of presented facts in such a way as to guide action towards a desired goal.” Today, the definition is still applicable but is now aided by various supporting IT applications.
BI can quickly get complex due to the many different inter-relationships between data and viewing the inter-relationships over longer periods of time (e.g., multiple years, etc.). Putting together the right relationships that are important to a radiology group will take time and detailed analysis. Once the data models are defined and the BI analytical tools are configured, gaining access to the data is essential.
Each of the above reporting solutions can create real strategic vantage points for radiology groups and departments. Aligning operational plans and strategic objectives to the most current, relevant information will keep the operations nimble and on-target. In each of these three operational and workflow metric solutions, however, they are only as good as the data available.
Gaining access to the right data flows is one challenge and then getting it at the right time and in the right format is another. Having an integrated workflow with the right supporting integration platform will lead to more effective real-time dashboard, operational reporting, and business intelligence implementations. This point is especially true when reading from multiple worklists and/or across multiple organizations.
Physician outreach
Connected care communities usually translate into Health Information Exchanges (HIE), Regional Health Information Organizations (RHIO), and/or a hub-and-spoke patient data exchange with a specific radiology practice as the center. For a radiology group, it comes down to having strong ties to the referring physician community, accepting patient orders, and delivering patient reports electronically.
Radiology groups with a robust integration platform are building their own interfaces through VPN connectivity to EMRs. With the proliferation of EMRs and the promise of incentives for their use, the demand from referring physicians for order and results interfaces is poised to grow. As the need to extend this service continues to grow, many groups may find it impractical to manage VPNs for external connectivity and will turn to web services solutions. The right supporting integrated workflow platform will ensure the radiology group has the capability to extend its reach effectively.
Review
Many times, the focus is creating strategic vantage points without putting the necessary foundation in place first.
There are countless analogies to use in underscoring the importance of starting with a robust foundation, yet there are many stories where this step is skipped or minimized. The strategic applications take the first look while the integrated workflow infrastructure is often overlooked. However, without the integrated workflow infrastructure in place first, the cost of obtaining the strategic vantage points may subdue the actual value achieved by these initiatives and/or extend the time in which the value is finally realized.
A key point is that the integrated workflow infrastructure supporting the workflows and applications may deliver as much, if not more value, than the strategic vantage point initiatives. Furthermore, the underlying infrastructure raises the success levels of the strategic initiatives and lowers the risk factors during their implementation.
To realize these benefits, a rational model is necessary to realize the value of all the competing initiatives. The model is illustrated in Figure 4.
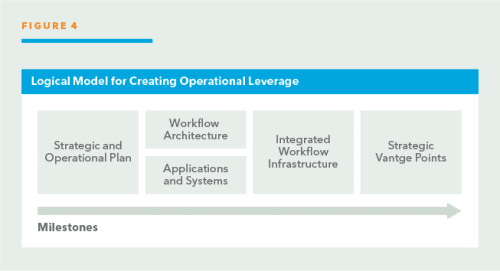
The key steps to implement a logical model are:
- Define and agree on a primary strategy and set goals for your radiology group or practice.
- Implement an operational plan to support the strategic goals.
- Define the workflow architecture and identify gaps with a plan to close them.
- Outline your workflows and define each critical touch point.
- Decide what applications and systems will play a role in orchestrating diagnostic volumes
- Define your integration approach to support the workflow architecture with respect to your referring physician connectivity objectives and approach.
- Leverage the support infrastructure to create strategic advantage and differentiating factors for your radiology group or department.
With a systematic approach to building strategic vantage points, greater value can be realized earlier in the process and costs can be lowered in implementing the new applications and systems.
